Abstract
Background:
Ruxolitinib (RUX), a JAK1/JAK2 inhibitor, and venetoclax (VEN), a BCL-2 inhibitor are 2 drug candidates recently identified as promising candidate for the treatment of T-Cell prolymphocytic leukemia (T-PLL). We recently reported that JAK/STAT pathway inhibition with RUX enhances BCL-2 dependence, thereby sensitizing T-PLL cells to VEN (Herbaux et al., Blood, 2021). We also showed that JAK/STAT pathway mutational status could impact RUX activity. Here, we report results on the 15 first patients who were treated with RUX and VEN oral combination for T-PLL. All patients were refractory to, or ineligible for alemtuzumab, the principal therapeutic option to date.
Methods:
In this multicenter retrospective study from the French Innovative Leukemia Organization, 15 patients with T-PLL (according to consensus criteria) were included. All patients were informed about the off-label use of this combination and provided informed consent. Patients received a maximum dose of RUX 15 mg twice daily, and VEN 800 mg daily. VEN was started with daily ramp-up from 20 mg to 800 mg over 6 days, with TLS prophylaxis (rasburicase and IV hydration). Responses were assessed by consensus criteria. Next generation sequencing (NGS) was performed using a custom-designed panel of 33 genes, including among others: ATM, TP53, IL2R, JAK1, JAK3, and STAT5B. CytoScan HD microarray (Affymetrix) were used to study copy number variation and or uniparental disomy. In vivo dynamic BH3 profiling (DBP) was performed on samples obtained from two patients on treatment.
Results:
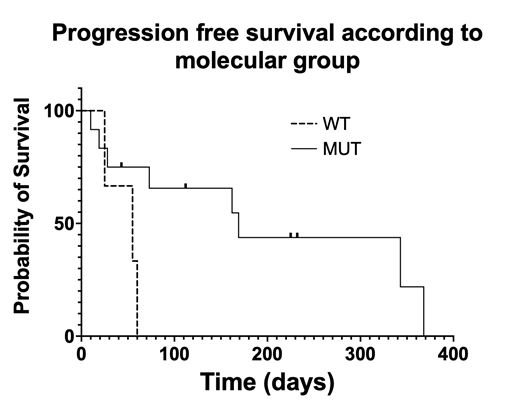
All 15 patients were refractory or relapsing after chemotherapy (mostly bendamustine and pentostatin), except one. They were either refractory to (n=10) or ineligible (n=5) for alemtuzumab (ineligibility was decided by the treating physician based on age and comorbidities). The median age was 70 years (48-88). Within a week of starting RUX, a transient increase of the absolute lymphocyte count was observed in 66.6% of the patients. Based on the molecular status of the JAK/STAT pathway, we established 2 groups of patients. One with samples where no mutations were found (WT, n=3), and one with at least one mutation in the JAK/STAT pathway (MUT, n=12). The overall response rate (ORR) was 73.3%, with only partial responses. Five patients nearly fulfilled CR criteria except that they had persistent lymphocytosis (over 4 x 10 9/L), all of them were in the MUT group. ORR was 83.3% in the MUT group, and only one patient of the WT group obtained a PR. With a median follow-up of 73 days (22 to 368), the median progression free survival was significantly shorter in the WT group in comparison to the MUT group (1.8 months versus 5.6 months, p=0.04, Figure). Of note, four patients were treated with VEN monotherapy before the start of the combination with RUX. With that treatment, 3 of these patients achieved stable disease followed by progression within 2 to 3 months, while 1 was primary refractory to VEN monotherapy. The most frequent reported adverse events (AEs) of the RUX plus VEN combination were cytopenias, with 46.6% grade 3 or 4 thrombocytopenia and 40% grade 3 or 4 neutropenia. DBP showed that overall priming and BCL2 dependence increased in vivo (n=2) during the treatment with RUX and VEN. Finally, SNP arrays identified clonal evolution in the 3 patients evaluated sequentially (before treatment versus at progression). In one case, emergence of EZH2 and JAK1 mutation was also observed at progression using NGS.
Conclusions:
These preliminary results suggest promising activity of RUX plus VEN in T-PLL, and justify the development of a prospective clinical trial of this combination. Our data seem to show that this combination may be especially active for patients with JAK/STAT pathway activating mutations and that disease progression is associated with clonal evolution. Updated results will be presented at the meeting.
Herbaux: Janssen: Honoraria; Roche: Honoraria; Abbvie: Honoraria, Research Funding; Takeda: Honoraria, Research Funding. Lemonnier: Gilead: Other: travel grant; Institut Roche: Research Funding. Laribi: Jansen: Research Funding; AstraZeneca: Other: Personal Fees; Takeda: Other: Personal Fees, Research Funding; Novartis: Other: Personal Fees, Research Funding; Astellas Phama, Inc.: Other: Personal Fees; IQONE: Other: Personal Fees; AbbVie: Other: Personal Fees, Research Funding; Le Mans Hospital: Research Funding; BeiGene: Other: Personal Fees. Moreaux: Diag2Tec: Consultancy. Morschhauser: Janssen: Honoraria; Servier: Consultancy; Incyte: Membership on an entity's Board of Directors or advisory committees; Epizyme: Consultancy, Membership on an entity's Board of Directors or advisory committees; AbbVie: Consultancy, Membership on an entity's Board of Directors or advisory committees; Celgene: Membership on an entity's Board of Directors or advisory committees; AstraZenenca: Membership on an entity's Board of Directors or advisory committees; BMS: Consultancy, Membership on an entity's Board of Directors or advisory committees; Chugai: Honoraria; Genentech, Inc.: Consultancy; Gilead: Consultancy, Membership on an entity's Board of Directors or advisory committees; Novartis: Consultancy, Membership on an entity's Board of Directors or advisory committees; Roche: Consultancy, Speakers Bureau; F. Hoffmann-La Roche Ltd: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees; Genmab: Membership on an entity's Board of Directors or advisory committees. Davids: Ascentage Pharma: Consultancy, Research Funding; MEI Pharma: Consultancy, Research Funding; Merck: Consultancy; Eli Lilly and Company: Consultancy; Adaptive Biotechnologies: Consultancy; Pharmacyclics: Consultancy, Research Funding; BMS: Consultancy, Research Funding; Research to Practice: Consultancy; BeiGene: Consultancy; Surface Oncology: Research Funding; Verastem: Consultancy, Research Funding; TG Therapeutics: Consultancy, Research Funding; Takeda: Consultancy; Astra-Zeneca: Consultancy, Research Funding; Novartis: Consultancy, Research Funding; Celgene: Consultancy; AbbVie: Consultancy; Genentech: Consultancy, Research Funding; Janssen: Consultancy; MEI Pharma: Consultancy. Ysebaert: Abbvie, AstraZeneca, Janssen, Roche: Other: Advisory Board, Research Funding.
Ruxolitinib and venetoclax are used offlabel for patients refractory to current therapeutic options, based on preclinical data.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal